Tendinopathy: Causes, Symptoms, Treatment and Exercises
 A tendon is a tough band of fibrous connective tissue made of collagen fibres that connect muscle to bone. They transmit forces from muscle to bone and as such have to be capable of withstanding tension. Due to the pressure we often put on our tendons to withstand great tensile stresses, tendon injuries are among the most common overuse injuries we see in the clinic.
A tendon is a tough band of fibrous connective tissue made of collagen fibres that connect muscle to bone. They transmit forces from muscle to bone and as such have to be capable of withstanding tension. Due to the pressure we often put on our tendons to withstand great tensile stresses, tendon injuries are among the most common overuse injuries we see in the clinic.
Tendinopathy is a broad term for a tendon injury with damage to the collagen fibres. Tendinitis (or tendonosis) is inflammation of the tendon. Research has suggested little or no long-term inflammation in tendon injuries and as such the term tendinopathy is now more commonly used.
Clinical presentation of patients with tendinopathies include:
- Pain
- Swelling
- Local tenderness and/or thickening
- Loss of flexibility
- Loss of strength
What Causes a Tendinopathy?
 Tendinopathies are caused by overuse or sudden stress on a tendon. As the strain on a tendon increases, tissue damage begins. With increased stress, some tendon fibres begin to fail which results in micro-tearing and ultimately tendon failure occurs. Histologist examination of these tendons shows separation and disarray of collagen bundles, increased poor quality blood vessels (neovascularization), increased cellular activity and inflammation.
Tendinopathies are caused by overuse or sudden stress on a tendon. As the strain on a tendon increases, tissue damage begins. With increased stress, some tendon fibres begin to fail which results in micro-tearing and ultimately tendon failure occurs. Histologist examination of these tendons shows separation and disarray of collagen bundles, increased poor quality blood vessels (neovascularization), increased cellular activity and inflammation.
How Can Physiotherapy, Chiropractic and Massage Therapy Help with Tendinopathy?
The first line of treatment for a tendinopathy injury is conservative management. A physiotherapist, chiropractor or massage therapist can help by tailoring a rehabilitation program to progress you from pain to performance. The first aim of managing tendinopathies is often to reduce pain and inflammation (if acute/reactive tendinitis). The key factor in reducing pain is managing the load on the tendon. The patient should avoid aggravating activities and any other excessive forces put on the tendon. Other treatment methods that can help with pain and inflammation include acupuncture/dry needling, therapeutic modalities (IFC, ultrasound), soft tissue releases, taping, exercise, and anti-inflammatory medication.
Your Physiotherapist and or Chiropractor will assess you and identify any movement dysfunctions or imbalance such as joint range of motion, muscle weakness, soft tissue tightness, poor control of movement, abnormal biomechanics and training errors. The identified dysfunction can be treated with a combination of hands on manual therapy or manipulation, soft tissue release, acupuncture/dry needling, and prescription of an individualized exercise program. Education in regards to lifestyle modification and training errors such as excessive training volume, intensity, inadequate recovery, footwear leading to poor biomechanics, training surface (concrete, hills.etc.) is also imperative.
Your Physiotherapist and or Chiropractor might also suggest extracorporeal shock wave therapy (ESWT) to treat your tendinopathy. There is research to suggest shockwave therapy can stimulate the healing process by breaking down scar tissue, realigning the collagen fibres, and stimulating an increased blood flow to the area.
What Should be Avoided with a Tendinopathy Injury?
You should avoid pushing through pain, quick movements and continuing to aggravate the tendon. You may feel better after warming up and stretching the area but it is still not recommended that you push through pain as you are risking further tissue damage delaying the healing process. Tendons are sensitive to overload so it is important you allow a proper amount of time for the tendon to heal.
How Long Does it Take to Recover from a Tendinopathy?
Recovery times differ (few weeks up to months) depending on the cause, severity, duration, area of injury, the integrity of the tendon and compliance with a rehabilitation program. Tendinopathies often take a long time to resolve particularly if symptoms have been present for some months before presentation. It is imperative to seek a qualified health care professional to treat the tendon and correct any associated dysfunctions that may have caused the tendinopathy. If your injury does not respond to conservative management, your physiotherapist will direct you to a physician for further investigation and treatment options.
What are Some Safe Home Exercises I can do for a Tendinopathy
The development of a home exercise program for an individual with tendinopathy requires clinical reasoning with consideration of the diagnosis and the functional requirements of the person. Exercise prescription will vary considerably depending on the site of the pathology (insertional or mid tendon), stage of tendinopathy (reactive or degenerative), functional assessment, contributing issues throughout the kinetic chain, and exercise/sport demands.
Once the pain has settled one of the goals of the exercise program will be to improve strength and function. Depending on your unique needs (ie. sport requirements) a physiotherapist will tailor the exercise program with the goal to gradually increase the load on the muscle and tendon while monitoring pain. Tendinopathy loading programs can include eccentric strengthening (loading as the muscle lengthens), combined (isometric, concentric and eccentric) or slow resistance training. Eccentric exercises have been considered the gold standard for many years, however, research has demonstrated the importance of also including the concentric phase of exercises. An example of eccentric loading involves slow lengthening muscle contractions such as the heel drop for the treatment of Achilles tendinopathy or wrist curls for tennis elbow:
Heel Drop Exercise
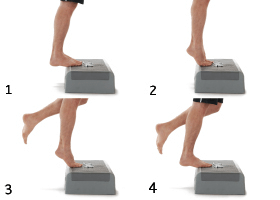
Elbow tendinopathy (tennis elbow) Exercises

Jumping Exercise

If you are suffering from tendinopathy and would like to see one of our experienced physiotherapists, chiropractors or registered massage therapists, please contact us today.
References:
- Scott et al. Conservative treatment of chronic Achilles tendinopathy. CMAJ 2011;183(10):1159-1165.
- Cook et al. The challenge of managing tendinopathy in competing athletes. Br J Sports Med 2014;48:506-509.
- Malliaras et al. Achilles and patellar tendinopathy loading programmes: a systematic review comparing clinical outcomes and identifying potential mechanisms for effectiveness. Sports Med 2013;43(4):267-286.
- Andres et al. Treatment of tendinopathy: what works, what does not, and what is on the horizon. Clin Orthop Relat Res 2008;466(7):1539-1554.
Rebalance Toronto
Rebalance Sports Medicine is a multidisciplinary clinic in downtown Toronto offering physiotherapy, chiropractic, registered massage therapy, sports medicine, naturopathy, Pilates and more.



 What to Expect From Your First Physiotherapy Visit
What to Expect From Your First Physiotherapy Visit The Benefits of Fascial Stretch Therapy [Demo]
The Benefits of Fascial Stretch Therapy [Demo] How Does Physiotherapy Work?
How Does Physiotherapy Work? Best Exercises for Low Back Pain
Best Exercises for Low Back Pain